
Advanced Surgical & Multidisciplinary Care by Dr. Lovedeep Singh Chauhan
Bladder cancer is a potentially serious yet highly treatable disease when diagnosed early and managed with the right expertise. Modern cancer care goes far beyond surgery alone — it requires accurate staging, evidence-based treatment planning, multidisciplinary coordination, and long-term surveillance.
Dr. Lovedeep Singh Chauhan , Consultant Surgical Oncologist in punjab at Max Super Speciality Hospital, provides comprehensive, guideline-directed management of bladder cancer with a focus on oncological safety, organ preservation when possible, and quality of life after treatment. This page offers detailed information about bladder cancer, its causes, symptoms, diagnosis, staging, and treatment options, followed by how specialized surgical oncology care can make a meaningful difference in outcomes.
Understanding Bladder Cancer
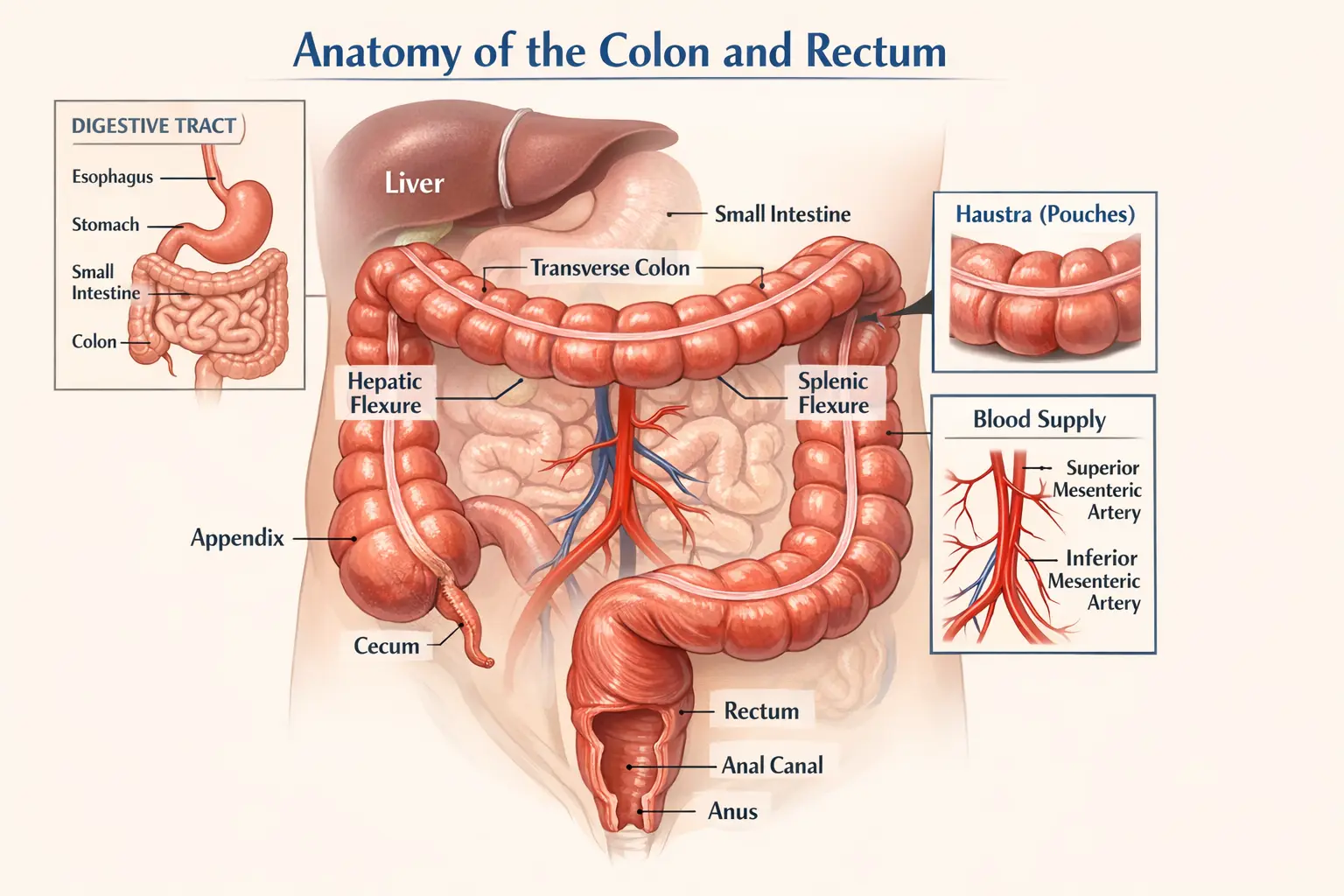
The urinary bladder is a hollow muscular organ located in the pelvis that stores urine before it is expelled from the body. The inner lining of the bladder is composed of specialized cells called urothelial cells. In most cases, bladder cancer begins in these lining cells and is therefore known as urothelial carcinoma (also called transitional cell carcinoma).
Bladder cancer can behave very differently depending on how deeply it invades the bladder wall. Some tumors remain superficial and are confined to the inner lining, while others penetrate the muscular layer and may spread to nearby lymph nodes or distant organs.
Types of Bladder Cancer
Urothelial Carcinoma
The most common type of bladder cancer, originating from the lining urothelial cells.
Squamous Cell Carcinoma
Often associated with chronic bladder irritation or infection.
Adenocarcinoma
A rare form arising from glandular cells of the bladder.
Small Cell Carcinoma
An aggressive and uncommon variant of bladder cancer.
Non-Muscle Invasive Bladder Cancer (NMIBC)
Tumors limited to the inner lining or just beneath it; common but prone to recurrence.
Muscle-Invasive & Metastatic Bladder Cancer
Cancers that invade the muscular layer or spread to distant organs; require aggressive treatment.
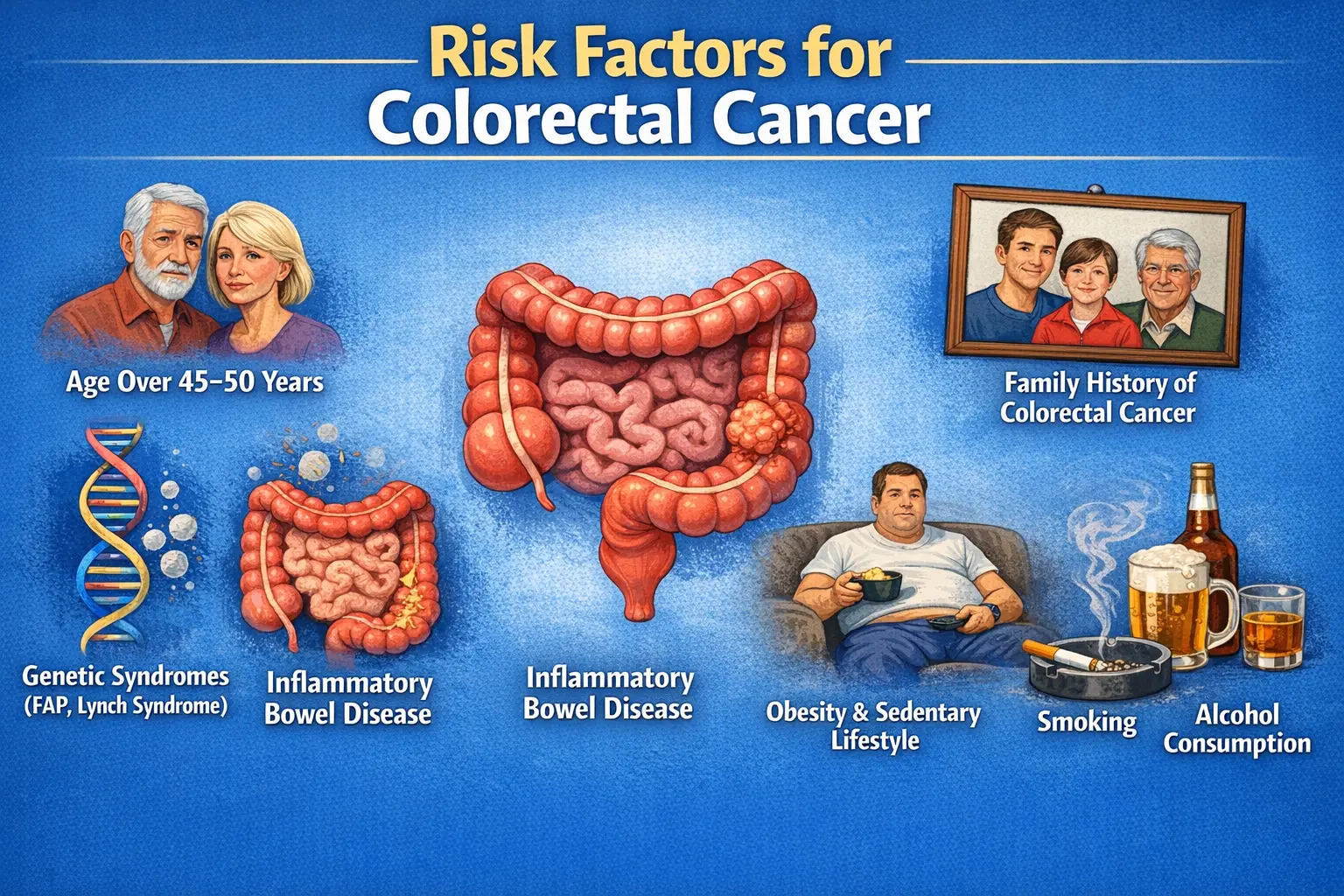
Risk Factors for Bladder Cancer
Smoking
Smoking is the single most important risk factor. Chemicals in tobacco are filtered by the kidneys and accumulate in urine, directly affecting the bladder lining.
Occupational Exposure
Long-term exposure to industrial chemicals used in dye, rubber, textile, leather, and paint industries increases bladder cancer risk.
Chronic Bladder Irritation
Repeated urinary infections, long-term catheter use, or bladder stones may contribute to bladder cancer development.
Prior Radiation Therapy
Radiation to the pelvis for other cancers can increase long-term risk of bladder cancer.
Age and Gender
Bladder cancer is more common in older adults and occurs more frequently in men.
Symptoms of Bladder Cancer
Early recognition of symptoms allows timely diagnosis and effective management.
The most common symptom of bladder cancer is painless blood in urine (hematuria). Even a single episode should never be ignored.
- Increased frequency of urination
- Burning sensation during urination
- Urgency to pass urine
- Pelvic discomfort
- Back pain (advanced cases)
- Unexplained weight loss (late stage disease)
Because these symptoms may resemble urinary infections, timely evaluation by a specialist is critical.
Diagnosis and Staging of Bladder Cancer
Accurate diagnosis and staging form the backbone of effective bladder cancer treatment. The evaluation typically includes:
Urine Tests
Urine analysis and cytology help detect abnormal cancer cells.
Ultrasound
A non-invasive imaging tool to detect masses within the bladder.
Cystoscopy
A thin camera is inserted through the urethra to visualize the bladder lining directly. Suspicious areas are biopsied.
TURBT
Transurethral Resection of Bladder Tumor is both diagnostic and therapeutic. The tumor is removed endoscopically and sent for histopathology.
CT Scan / MRI
These imaging studies assess tumor depth and check for lymph node involvement or distant spread.
TNM Staging
Bladder cancer staging is based on Tumor depth (T), Lymph node involvement (N), and Metastasis (M). Correct staging ensures optimal treatment.
Treatment of Non-Muscle Invasive Bladder Cancer
Non-muscle invasive tumors are often treated successfully with endoscopic management. Early-stage disease, when managed appropriately, has excellent long-term survival outcomes.
TURBT
The first step involves complete removal of visible tumor through TURBT. The quality of this procedure significantly influences recurrence rates.
Intravesical Therapy
In selected patients, medication is instilled directly into the bladder. BCG (Bacillus Calmette-Guérin) is commonly used to reduce recurrence and progression risk.
Surveillance
Because superficial bladder cancer has a high recurrence tendency, periodic cystoscopy is essential. Follow-up intervals are individualized based on risk category.
Treatment of Muscle-Invasive Bladder Cancer
When cancer invades the muscle layer, more aggressive treatment is necessary. Treatment decisions are personalized and based on international guidelines.
Radical Cystectomy
Surgery involves removal of the entire bladder along with surrounding lymph nodes. In men, the prostate may also be removed. In women, adjacent reproductive organs may be involved depending on extent.
Urinary Diversion Options
After bladder removal, urine needs a new pathway:
• Ileal conduit (external stoma with urine bag)
• Orthotopic neobladder (internal bladder reconstruction using intestine)
• Continent diversion pouch
Choice depends on patient suitability, tumor factors, and overall health.
Chemotherapy
Neoadjuvant chemotherapy (before surgery) improves survival in muscle-invasive disease. In selected cases, adjuvant therapy may also be advised.
Bladder Preservation Protocol
In carefully selected patients, combined chemotherapy and radiation may preserve the bladder.
Management of Advanced and Metastatic Bladder Cancer
When bladder cancer spreads beyond the bladder, systemic treatment becomes the cornerstone of management. Even in advanced disease, symptom control and supportive care are essential for maintaining dignity and comfort.
Systemic Treatment Options
- Combination chemotherapy
- Immunotherapy
- Targeted therapy
- Palliative interventions to improve quality of life
Importance of Multidisciplinary Care
- Surgical oncology
- Medical oncology
- Radiation oncology
- Radiology
- Pathology
- Stoma care specialists
- Tumor board discussions help determine the best evidence-based treatment plan
Surgical Expertise of Dr. Lovedeep Singh Chauhan
Dr. Lovedeep Singh Chauhan is a trained Surgical Oncologist with advanced expertise in complex oncologic procedures. His approach to bladder cancer emphasizes evidence-based, patient-centered care.
Minimally Invasive Surgical Approaches
- Smaller incisions
- Reduced blood loss
- Faster recovery
- Shorter hospital stay
- Surgical approach selected based on tumor stage and patient suitability
Recovery After Bladder Cancer Surgery
- TURBT: rapid recovery, resume normal activities within days
- Radical cystectomy: hospital stay ~1 week
- Gradual return to activity over 4–6 weeks
- Education on stoma care (if applicable)
- Nutritional counseling
- Structured follow-up plan for recurrence monitoring and long-term health
When Should You Consult a Specialist?
Early evaluation is essential for better outcomes. Seek immediate attention if you notice any of the following:
- Any episode of blood in urine
- Recurrent urinary infections
- Persistent urinary urgency without infection
- Pelvic pain or unexplained weight loss
Why Choose Specialized Surgical Oncology Care?
Bladder cancer treatment is complex and demands more than technical skill. It requires a combination of expertise, experience, and patient-centered care to achieve optimal outcomes.
- In-depth understanding of tumor biology
- Experience in complex pelvic surgery
- Multidisciplinary coordination
- Personalized decision-making
- Compassionate communication
Dr. Lovedeep Singh Chauhan combines academic training, surgical precision, and patient-focused care to ensure treatment aligns with global oncologic standards.


